Cancer Plan Minnesota
Goal 2: Prevention


Prevent cancer before it starts.
Imagine a Minnesota where far fewer people face a cancer diagnosis. While not every cancer can be prevented, some are linked to modifiable risk factors like commercial tobacco use, poor nutrition, limited physical activity, alcohol use, and exposure to harmful substances in our environment. Prevention relies heavily on access, opportunity, and community conditions. Some Minnesotans live in communities where it is hard to find healthy food, safe places to be active, clean air and water, or affordable cancer-preventing vaccines. Some face regular exposure to cancer-causing agents like radon, ultraviolet radiation, or other environmental toxins.
Cancer Plan Minnesota includes strategies to address these challenges at their roots by creating healthier environments, improving access to prevention resources, and removing barriers to lasting change.
Objectives
- 2.1: Culturally responsive prevention
- 2.2: Commercial tobacco*
- 2.3: Nutrition & physical activity
- 2.4: Alcohol-related cancer risk
- 2.5: Radon exposure
- 2.6: Other environmental exposures
- 2.7: HPV vaccination
- 2.8: Hepatitis B vaccination
- 2.9: Ultraviolet (UV) exposure
2.1: Culturally responsive prevention
Reduce cancer incidence and mortality among communities disproportionately impacted by
cancer.
cancer.
Strategies:
- Identify community-level barriers to and opportunities for primary prevention.
- Conduct tailored outreach and education about cancer risk and opportunities for risk reduction.
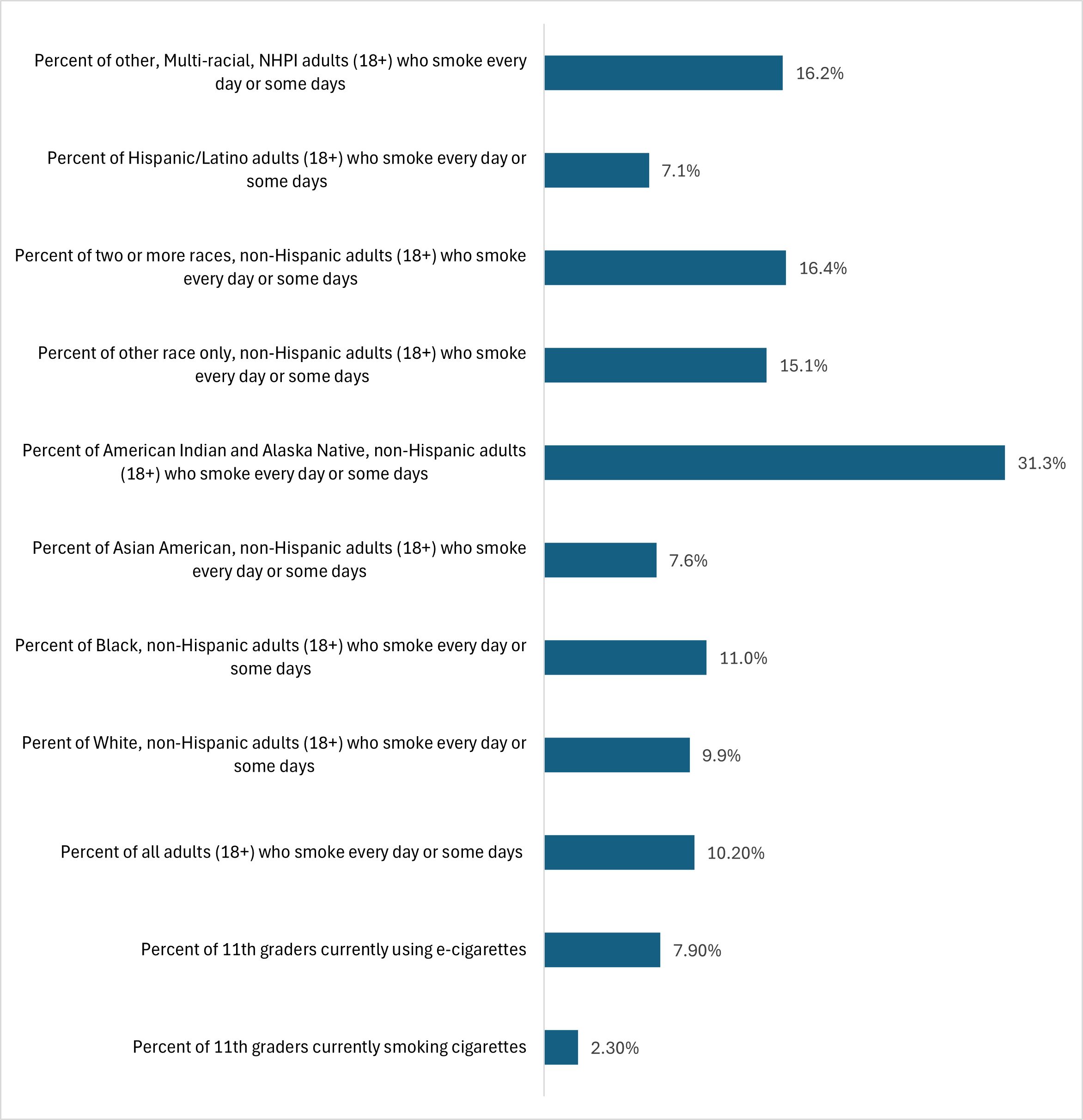
2.2: Commercial tobacco
Reduce the use of commercial tobacco* among adolescents and adults and address commercial tobacco-related racial and health disparities.
Strategies:
- Maintain data collection on commercial tobacco use and commercial tobacco-related disease from communities that have high rates of commercial tobacco use, employing sufficiently large and culturally appropriate sampling strategies.
- Partner with communities most impacted by commercial tobacco to develop and implement community-driven solutions to eliminate nicotine dependence.
- Conduct outreach and education about traditional tobacco versus commercial tobacco.
- Advocate for policies that fund commercial tobacco prevention and treatment, limit access and appeal of commercial tobacco products, maintain high prices for commercial tobacco products, and promote smoke-free air.
- Advocate for policies and implement programs that build on youth e-cigarette prevention and cessation initiatives.
- Engage and partner with healthcare providers and health systems to embed commercial tobacco screening protocols using brief intervention and referral to the Quit Partner and other treatment options.
*Commercial tobacco in this report refers specifically to the use of manufactured, commercial tobacco products, and not to the sacred, medicinal, and traditional use of tobacco by American Indians and other groups. Commercial tobacco includes cigarettes, cigars, e-cigarettes, hookah, nicotine pouches, and other smokeless tobacco products.
2.3: Nutrition and physical activity
Increase access to healthy food and physical activity among children and adults.
Strategies:
- Identify communities with lower access to healthy food and fewer opportunities for physical activity.
- Strengthen relationships with partners working on nutrition and physical activity.
- Advocate for policies and implement programs that increase opportunities for safe, easy, and effective places for people to be physically active.
- Implement programs that increase access to safe, nutritious, and culturally-appropriate food.
- Advocate for policies that reduce consumption of sugar-sweetened beverages.
2.4: Alcohol-related cancer risk
Decrease alcohol consumption and heavy alcohol use among adolescents and adults.
Strategies:
- Identify communities disproportionately impacted by alcohol-related harms and/or higher-risk drinking patterns.
- Support alcohol use screening protocols using a brief intervention model and referral to rehabilitation and treatment when appropriate.
- Raise awareness of cancer risk associated with alcohol use, tailored to communities disproportionately impacted by alcohol-related harms.
- Advocate for policies that reduce the affordability of and access to alcohol.
2.5: Radon exposure
Decrease exposure to radon.
Strategies:
- Identify communities disproportionately impacted by radon exposure.
- Partner with community-based organizations to promote testing and mitigation.
- Conduct tailored outreach and education to inform communities about radon exposure as a risk factor for cancer and options for testing and mitigation.
- Advocate for policies that protect communities from radon exposure and reduce barriers to testing and mitigation.
2.6: Other environmental exposures
Reduce exposure to environmental carcinogens.
Strategies:
- Identify communities disproportionately impacted by environmental carcinogens.
- Partner with community-based organizations to promote risk reduction.
- Conduct tailored outreach and education to inform communities about environmental exposures as risk factors for cancer and options for reducing exposure.
- Advocate for policies that protect communities from exposure to environmental carcinogens and reduce barriers to risk reduction.
2.7: HPV vaccination
Increase uptake and completion of the HPV vaccine series.
Strategies:
- Identify communities with unique challenges to vaccination uptake.
- Partner with community-based organizations to reduce vaccine hesitancy.
- Train healthcare providers on evidence-based practices to improve HPV vaccination uptake.
- Expand vaccination and education opportunities outside of the traditional clinic setting.
- Conduct tailored outreach and education to inform communities about vaccine-preventable cancers and opportunities for vaccination.
- Advocate for policies that increase HPV vaccination.
2.8: Hepatitis B vaccination
Increase uptake and completion of the Hepatitis B vaccine series.
Strategies:
- Identify communities with unique challenges to vaccination uptake.
- Partner with community-based organizations to reduce vaccine hesitancy.
- Train healthcare providers on evidence-based practices to improve Hep B vaccination uptake.
- Expand vaccination and education opportunities outside of the traditional clinic setting.
- Conduct tailored outreach and education to inform communities about vaccine-preventable cancers and opportunities for vaccination.
- Advocate for policies that increase Hep B vaccination.
2.9: Ultraviolet (UV) exposure
Reduce exposure to harmful UV radiation.
Strategies:
- Identify communities most impacted by sun exposure.
- Partner with community-based organizations, schools, and worksites to address sun exposure and protection.
- Promote shade planning and individual sun-protective behaviors in outdoor settings.
- Enforce and strengthen existing laws governing indoor tanning facilities.
- Advocate for workplace policies that protect outdoor workers from UV radiation.
